How The Birth Experience Is Owned By Technology
In his extraordinary chapter on the psychological aspects of childbirth in The Psychology of Birth (by Leslie Feher), Louis E Mehl systematically outlines the ways in which physicians in labour wards cope with anxiety: by splitting off from emotional relationship with the patient, and by depersonalising the birthing mother through standardised medical ritual procedures and clothing.
Mehl writes: ‘Childbirth is of central importance in every culture. Every society has fertility rites, birth myths and art, and persons whose duties to the community involve attending births. Because birth is so necessary for the preservation of society, childbirth practices tend to reflect the deepest values of the culture. This is true also for the other rites of passage, including the transition to adulthood, marriage and death, but birth has been more difficult to study anthropologically because it has usually been a private family-friend affair, whereas these other events tend to involve the entire community.’
Birth experience in the hospital
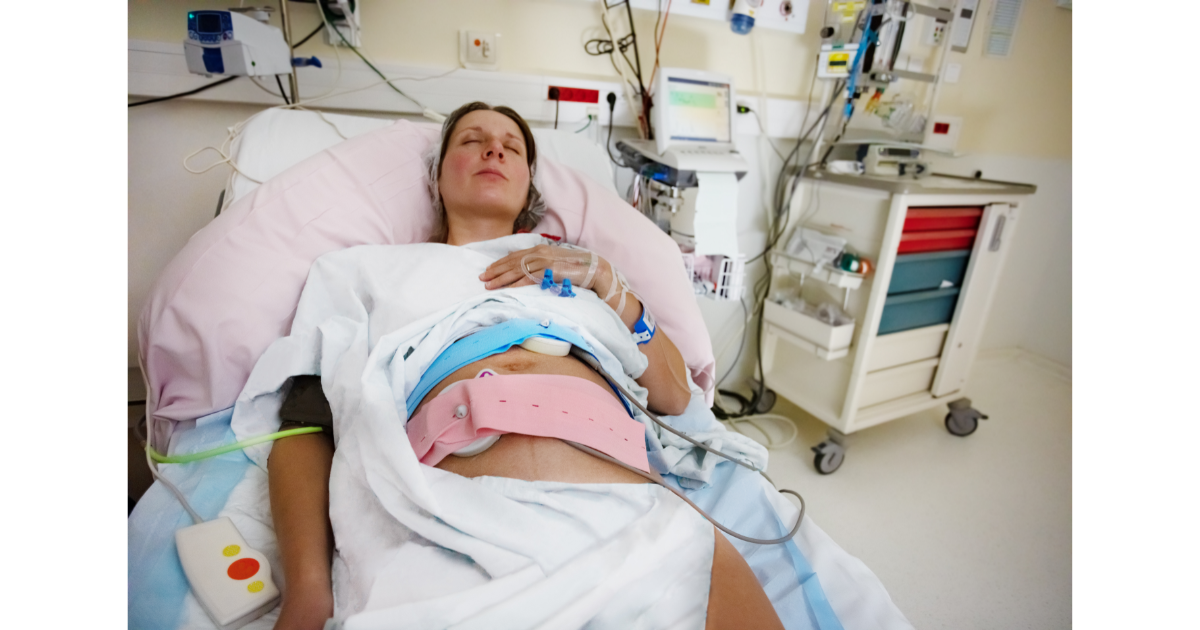
Birth has become a technical rather than an emotional experience in the same way as death – both take place within a sterile hospital atmosphere. Emotions have become controlled by chemicals rather than being expressed in a healing environment. The intimacy and emotional power of childbirth can be stripped away by the impersonal attitudes of hospital staff and the technical procedures they use.
In the West this depersonalisation has been regarded as progressive; however, these ostensibly progressive changes have a profound cultural impact on individuals and families. Making birth and death technical rather than significant life events is symptomatic of a deeper process of technological control over our lives.
The technologisation of the twentieth century has contributed to a move away from the traditional childbirth practices – home birth attended by a midwife – to birth in a hospital assisted by instruments and drugs. In this environment, the baby is separated from the mother and both are isolated from the family. Instead, they are surrounded by machines, routines, doctors, nurses, and an impersonal approach.
Obstetrics courses in medical schools ensure that the birth practices developed from the 1920s to the 1950s remain pervasive in the West. Allopathic medicine, which represents the medical model as we know it today, tends to ignore the psychological factors affecting health, as well as the traditional organic herbal remedies.
‘This allopathic tradition involves reliance on drugs and surgery to relieve symptoms, rather than more holistic techniques aimed at preserving health, via good exercise and a healthy lifestyle. Giving birth under this regime is a very sterile undertaking, literally and figuratively,’ according to Mehl.
Controlled birth
In the 50s, the woman came to the hospital early in labour. Once admitted, her pubic hair was shaved, she was given an enema, and often an intravenous solution. The course of birth was very lonely as her husband or support person was not allowed to be with her, not even in the labour room. During labour pain medication (such as meperidine (Pethidine), morphine, and Nysentil) was routinely administered. At the time of the pushing stage a general anaesthesia was given so the baby had to be delivered with forceps over a wide episiotomy.
Mehl describes the alienating atmosphere of the labour room: ‘During delivery, the woman was flat on her back on a delivery table with sterile drapes over everything except her vagina and perineum. Everyone present would be garbed in caps, masks, sterile suits and sterile operating garb. There was little place for humanity. Doctors and nurses would chatter, as they do during surgery, about sports and politics, well-spiced with sexual innuendos and sexual game-playing between doctor and nurse.’
‘Once the patient was under general anaesthesia, she would not infrequently be the object of humour or ridicule. After the birth, the baby would go to the nursery. The mother might not see her child for the first twenty-four hours, and thereafter only every four hours for feeding during the day.’
Birth experience and technology
Mehl also points out the conditioned cultural helplessness of birthing women, which is perpetuated by attitudes toward hospital births. ‘In routine technological delivery, it remains common for the woman to enter the hospital in very early labour – 2 cm cervical dilation – largely because she has never been adequately instructed about the feelings to expect. So she is put in bed and conditioned to a passive role, both physically and mentally. She spends hours lying around, as little happens to move labour along, whereas in fact walking and activity, and an active energised mind, are most useful for good labour to progress.’
Passivity is a common cause of failure of the uterus to contract effectively. Hence it becomes necessary to administer the hormone oxytocin to encourage contractions, with risks for mother and baby. A passive mental attitude also increases pain sensation: by focusing on pain it becomes more intense. This then leads to more passivity.
When hard labour finally begins, it is experienced more intensely than it otherwise might. Electronic foetal monitoring is common. To do this the amniotic sac (bag of waters) is ruptured, and a catheter pushed through the vagina and cervix past the head of the fetus into the uterus to record the strength of uterine contractions. Then a metal electrode is applied to the baby’s scalp to monitor the baby’s heart rate.
Mehl also is critical of the drugs given routinely to birthing women: ‘Pain relieving drugs are ordinarily given after 4 cm cervical dilation. Epidural anaesthesia may be given at 5 to 6 cm of cervical dilation. This is done by threading a catheter through a needle into the space around the dura (the covering of the spinal cord) in the low back area of the spine. The anaesthetic is infused through this catheter to bathe the nerves and cause numbness in the areas reached by them, including the abdomen and the lower legs. The ability to move is greatly diminished, and occasionally there is significant hypotension (low blood pressure) at the time of placement of the epidural. This can cause distress in the baby by decreasing the amount of blood (and therefore oxygen) received from the placenta. Spinal anaesthetics are similar to epidurals, but they involve more risk.’
Who benefits from medical interference?
Often the medical interference does not benefit the patient but the doctor or medical students: ‘In some hospitals, it is routine practice for all women having their first child to be given epidural anaesthesia and to have a forceps delivery. This can be simply because the resident physicians (registrars) want more training and experience in the use of forceps.
The residents (registrars) and nurses encourage the woman to accept drugs and epidural anaesthesia by telling them how good it will feel to be free of the pain, and that it will not harm the baby in any way. This constitutes a powerful indirect hypnotic suggestion.
After delivery, the mother then feels she could not have given birth without the aid of forceps and medical intervention, not realising that the anaesthesia made her unable to push and therefore necessitated the use of forceps.’
The medicalisation of the birth experience
The medicalisation of childbirth as a social tool teaches women a dependent, patient role. This process could be called indirect hypnosis. According to Mehl, it is ‘a powerful means of convincing women who are in a naturally vulnerable state while in labour that unnecessary procedures are essential so that they in turn become grateful to the physician-rescuer. The essence of such socialisation is the creation of a class of women willing to allow their births to be controlled by technology.’
However, not only birth but also other natural transitions in a woman’s life are thus medicalised: menstruation, family planning, and menopause. ‘In this way, women become socialised into being dependent upon physicians and the medical establishment to cope with their normal, natural physiological functions.’
There is now a growing movement to humanise childbirth – women demanding control over their own labour, the emotional support of their families rather than anaesthesia to deal with pain, and immediate contact with their babies.
While not negating pain, Mehl advocates birth as a positive experience: ‘At its most self-aware, the new consciousness accepts the painful aspect of parturition and assents that pleasure can exist parallel to pain, insisting on complete sentience and even finding childbearing a transcendental experience, ecstatic to the mother and, perhaps, also for the child. There is a growing concern with how to make the birth experience a source of profound personal growth for the mother and a psychologically/ spiritually positive experience for the infant.’




